Consider this: Right now, as youŌĆÖre sitting there, thereŌĆÖs a battle raging in your belly. Some 1,000 species of bacteria are duking it out, trying to establish dominance. Why should you care? Because whether the good bacteria in your gut or the bad triumph doesnŌĆÖt just decide how well you digest your dinner, respond to allergens and fend off diseasesŌĆöit also helps determine how much weight youŌĆÖre likely to gain. Or lose.
ŌĆ£Simply put, if you get the microbiomeŌĆöthat collection of bacteria inside youŌĆöhealthy, you will lose weight,ŌĆØ says Raphael Kellman, MD, a New York City physician and author of┬ĀThe Microbiome Diet.┬ĀŌĆ£ItŌĆÖs less about eating a certain percentage of carbohydrates, protein and fat than about correcting the overgrowth of unhealthy bacteria, which is making you crave the wrong foods, triggering inflammation.ŌĆØ
What exactly is ŌĆ£the gutŌĆØ?
Our gut is home to approximately┬Ā100,000,000,000,000 (100 trillion) microorganisms. ThatŌĆÖs such a big number our human brains canŌĆÖt really comprehend it.┬ĀOne┬Ātrillion dollar bills laid end-to-end would stretch from the earth to the sun ŌĆō and back ŌĆō with a lot of miles to spare. Do that 100 times and you start to get at least a vague idea of how much 100 trillion is.
 The human gut contains 10 times more bacteria than all the human cells in the entire body, with over 400 known diverse bacterial species. In fact, you could say that┬ĀweŌĆÖre more bacterial than we are human. Think about that one for a minute.
The human gut contains 10 times more bacteria than all the human cells in the entire body, with over 400 known diverse bacterial species. In fact, you could say that┬ĀweŌĆÖre more bacterial than we are human. Think about that one for a minute.
WeŌĆÖve only recently begun to understand the extent of the gut floraŌĆÖs role in human health and disease. Among other things, the gut flora promotes normal gastrointestinal function, provides protection from infection, regulates metabolism and comprises more than 75% of our immune system. Dysregulated gut flora has been linked to diseases ranging from autism and depression to autoimmune conditions like HashimotoŌĆÖs, inflammatory bowel disease and type 1 diabetes.
Recent research has shown that the gut flora, and the health of the gut in general, also play a significant role in both obesity and diabetes. IŌĆÖve seen this anecdotally in my practice as well. Nearly every patient I treat with a blood sugar issue also has a leaky gut, a gut infection, or some other chronic inflammatory gut condition.
We now know that the composition of the organisms living in your gut determines ŌĆō to some extent, at least ŌĆō how your body stores the food you eat, how easy (or hard) it is for you to lose weight, and how well your metabolism functions. LetŌĆÖs take a closer look at the mechanisms involved.
Intestinal bacteria drive obesity and metabolic disease
A study published this year in Science magazine found that mice without a protein known as toll-like receptor 5 (TLR5) in their gut gain excessive weight and develop full-blown diabetes and fatty liver disease when fed a high-fat diet. If we think of the gut flora as a community, TLR5 is like a neighborhood police force that can keep the houligans in check. Without TLR5, bad bacteria can get out of control.
The study authors found that these bad bacteria caused a low-grade inflammation in the mice, which caused them to eat more and develop insulin resistance. They also found that treating these mice with strong antibiotics (enough to kill most of the bacteria in the gut) reduced their metabolic abnormalities.
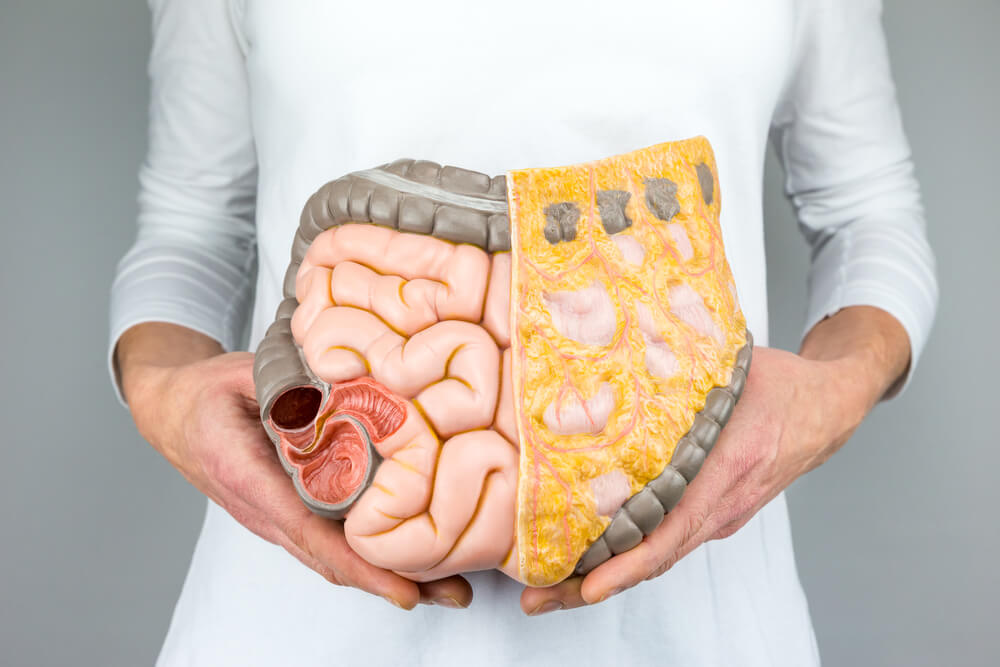
But the most interesting part of this study is what happened when the researchers transferred the gut flora from the TLR5-deficient overweight mice into the guts of skinny mice: the skinny mice immediately started eating more and eventually developed the same metabolic abnormalities the overweight mice had. In other words, obesity and diabetes were ŌĆ£transferredŌĆØ from one group of mice to the other simply by changing their gut flora (as shown in the image below).
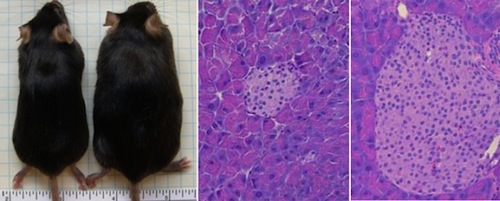
In the study on TLR5 deficient mice mentioned above, the mice with too much bad bacteria in their guts experienced an increase in appetite and ate about 10 percent more food than their regular relatives. But it wasnŌĆÖt just that these mice were hungrier and eating more; their metabolisms were damaged. When their food was restricted, they lost weight ŌĆō but still had insulin resistance.
Other studies have shown that the composition of the gut flora differs in people who are obese and diabetic, and people who are normal weight with no metabolic irregularities.
One possible mechanism for how changes in the gut flora cause diabesity is that different species of bacteria seem to have different effects on appetite and metabolism.
A flurry of ground-breaking findings are helping to connect the dots about how our gut bacteria may shape our, well, shape. In a study in the┬ĀBritish Journal of Nutrition,┬Āobese women who took a probiotic supplement (of the bacteria Lactobacillus rhamnosus) lost twice as much weight and fat over about six monthsŌĆöand were better at keeping it offŌĆöas those who took a placebo. Probiotics may have helped by controlling the womenŌĆÖs appetites, which seem to have waned as their microbiomes changed.
Unhealthy gut bacteria also produce food cravings: A study published in┬ĀBioEssays┬Āsuggests that some microbes may drive us to eat doughnuts or another tempting treat. These gut bugs send chemical messages to the brain that sway our appetite and moodŌĆöperhaps making us feel anxious until we gobble a square of dark chocolate or a T-bone steak.
Other studies have shown that changes in the gut flora can increase the rate at which we absorb fatty acids and carbohydrates, and increase the storage of calories as fat. This means that someone with bad gut flora could eat the same amount of food as someone with a healthy gut, but extract more calories from it and gain more weight.
Bad bugs in the gut can even directly contribute to the metabolic syndrome by┬Āincreasing the production of insulin (leading to insulin resistance), and by causing inflammation of the hypothalamus (leading to leptin resistance).
Modern life: screws up our gut and makes us fat and diabetic
What all of this research suggests is that┬Āhealthy gut bacteria is crucial to maintaining normal weight and metabolism. Unfortunately, several features of the modern lifestyle directly contribute to unhealthy gut flora:
ŌĆō Antibiotics and other medications like birth control and NSAIDs
ŌĆō Diets high in refined carbohydrates, sugar and processed foods
ŌĆō Diets low in fermentable fibers
ŌĆō Dietary toxins like wheat and industrial seed oils that cause leaky gut
ŌĆō Chronic stress
ŌĆō Chronic infections
We also know that infants that arenŌĆÖt breast-fed and are born to mothers with bad gut flora are more likely to develop unhealthy gut bacteria, and that these early differences in gut flora may predict overweight and obesity in the future.
ItŌĆÖs interesting to note that the diabesity epidemic has neatly coincided with the increasing prevalence of factors that disrupt the gut flora. IŌĆÖm not suggesting that poor gut health is the single cause of obesity and diabetes, but I am suggesting that┬Āit likely plays a much larger role than most people think.
How is Your Gut?
Despite whether or not you already eat relatively healthy, your gut may still be a little out of whack. HereŌĆÖs how to check:
Gut check #1: Get Your Two PŌĆÖs
Basically, it all begins with probiotics and prebiotics, components of food believed to play an important role in improving gut health.┬ĀProbiotics┬Āare a type of good bacteria, similar to the ones that already reside in your gut. Ingesting these organisms aids digestion┬Āand┬Āhelps change and repopulate intestinal bacteria to balance what doctors refer to as ŌĆ£gut flora.ŌĆØ┬ĀPrebiotics┬Āare plant-fiber compounds, also found in food, that pass undigested through the upper part of the gastrointestinal tract and help stimulate the growth of good bacteria. When pre- and probiotics are combined, they become an intestinal power couple (or, in blunter terms, they kick nutritional butt).
Gut check #2: Go Live
Fermented foods deliver probiotics directly to the gut. A cup of yogurt a day? ItŌĆÖs a nice start. Look for products that say ŌĆ£live and active culturesŌĆØ on the label, and be careful when it comes to fruit-infused flavors: Some are loaded with sugar, which can feed bad bugs, so be sure to check the ingredients and aim for fewer than 15 grams per serving. For even more probiotics, try Greek yogurt or kefir, a tangy dairy drink thatŌĆÖs packed with good bugs. A 2011 Harvard study found that yogurt was more strongly linked to weight loss than any other health food. In fact, people who ate an extra serving a day lost nearly a pound every four years.
Gut check #3: Down Some Fiber
It does more than fill you up: Research shows that foods that are high in fiber help promote the growth of friendly bacteria. Case in point: In a University of Illinois study, people who ate high-fiber snack bars experienced a growth of anti-inflammatory bacteria in their bellies.
Gut check #4: Mix Up Your Menu
Eat an assortment of foods to encourage a more varied metropolis in your belly. Recent studies suggest that the intestines of lean people look more like bustling cities than sleepy towns. (Translation: TheyŌĆÖre densely populated and diverse.) One study showed that individuals who had a healthy weight, body mass index, waist circumference and blood sugar level were more apt to have high levels of three different types of bacteriaŌĆöFirmicutes, Bifidobacteria and Clostridium leptum. WhatŌĆÖs more, in a pair of French studies, people with diverse gut microbiomes were less likely to be obese or at risk of diabetes. Plus, their intestinal ecosystems were home to fewer pro-inflammatory bacteria. ItŌĆÖs easy to change up your meals: If you had salad with grilled chicken yesterday, for example, go with a fish taco or a tofu stir-fry today.
Gut check #5: Skip Bad-News Foods
What you donŌĆÖt eat is every bit as crucial as what you do add to your diet. Keep your gut flora fit by cutting back on these offenders.
Refined carbs
Fatty and sugary foods not only tend to lack fiberŌĆöwhich is ideal food for the microbiomeŌĆöbut can also cause bad bacteria to thrive. And letŌĆÖs face it: If youŌĆÖre pounding that bag of potato chips, chances are youŌĆÖre not munching on celery sticks, blueberries and other gut-friendly eats.
Animal protein
A diet heavy in fat and protein (such as meat and cheese) feeds a type of bacteria, Bilophilia, that has been linked to inflammation. Lawrence David, PhD, assistant professor at Duke UniversityŌĆÖs Institute for Genome Sciences and Policy, saw the levels of this bacteria shoot up in study participants scarfing ribs and brisket, but not in those eating squash and lentils. Dr. Kellman suggests limiting red meat to once a week. ItŌĆÖs smart for your heartŌĆöand hips!
How to maintain and restore healthy gut flora
The most obvious first step in maintaining a healthy gut is to avoid all of the things I listed above. But of course thatŌĆÖs not always possible, especially in the case of chronic stress and infections, and whether we were breast-fed or our mothers had healthy guts.
If youŌĆÖve been exposed to some of these factors, there are still steps you can take to restore your gut flora:
- Remove all food toxins from your diet
- Eat plenty of fermentable fibers (starches like sweet potato, yam, yucca, etc.)
- Take a high-quality probiotic, or consider more radical methods of restoring healthy gut flora
- Treat any intestinal pathogens (such as parasites) that may be present
- Take steps to manage your stress
Fortunately, we can begin to take control by feeding our microbiome the right foods. ŌĆ£I tell my patients, ŌĆśThe bacteria follow the food,’ŌĆØ says gastroenterologist Robynne Chutkan, MD, founder of the Digestive Center for Women in Chevy Chase, Md., and author of┬ĀGutbliss.ŌĆ£What we eat dictates the kind of bacteria we grow in our gut garden.ŌĆØ
This is big news: There are trillions of microbes in your belly that willŌĆöif you feed them wellŌĆöhelp you fight flab and win.
Sources:
http://www.health.com/health/article/0,,20859953,00.html
https://chriskresser.com/a-healthy-gut-is-the-hidden-key-to-weight-loss/